Medical billing is not a one-size-fits-all process. Each medical discipline has its own unique coding requirements, payer regulations, documentation standards, and reimbursement challenges. That’s why understanding medical billing specialties is crucial for healthcare providers who want to maintain compliance, reduce denials, and maximize revenue.
For healthcare practices across the USA, partnering with an experienced billing company like CareMSO can significantly improve operational efficiency and financial performance. In this comprehensive guide, we’ll explore specialty medical billing, why it matters, and how it impacts your practice’s revenue cycle.
What Are Medical Billing Specialties?
Medical billing specialties refer to billing and coding services tailored to specific healthcare disciplines. Each specialty uses unique CPT codes, ICD-10 codes, modifiers, and payer guidelines.
For example:
Cardiology billing differs significantly from dermatology billing.
Mental health billing involves distinct compliance and authorization rules.
Surgical specialties require precise global period tracking and modifier usage.
Because of these differences, specialty-specific expertise ensures accurate claim submission and faster reimbursements.
Why Specialty Medical Billing Matters in the USA
The U.S. healthcare system is highly regulated and insurance-driven. Medical practices must comply with:
Medicare regulations
Medicaid policies
Commercial insurance rules
HIPAA compliance standards
State-specific payer guidelines
Without specialty-focused billing knowledge, practices face:
Increased claim denials
Delayed reimbursements
Compliance risks
Revenue loss
Audit vulnerabilities
That’s why specialized billing solutions from CareMSO are essential for sustainable growth.
Common Medical Billing Specialties in the USA
Below are some of the most common medical billing specialties and what makes each unique.
1. Cardiology Billing
Cardiology billing involves complex diagnostic procedures such as:
Echocardiograms
Stress tests
Cardiac catheterization
Holter monitoring
Challenges:
Bundled services
Modifier 26 and TC usage
Medical necessity documentation
Prior authorizations
Accurate coding directly impacts high-value reimbursements.
2. Dermatology Billing
Dermatology includes both medical and cosmetic services.
Billing complexities include:
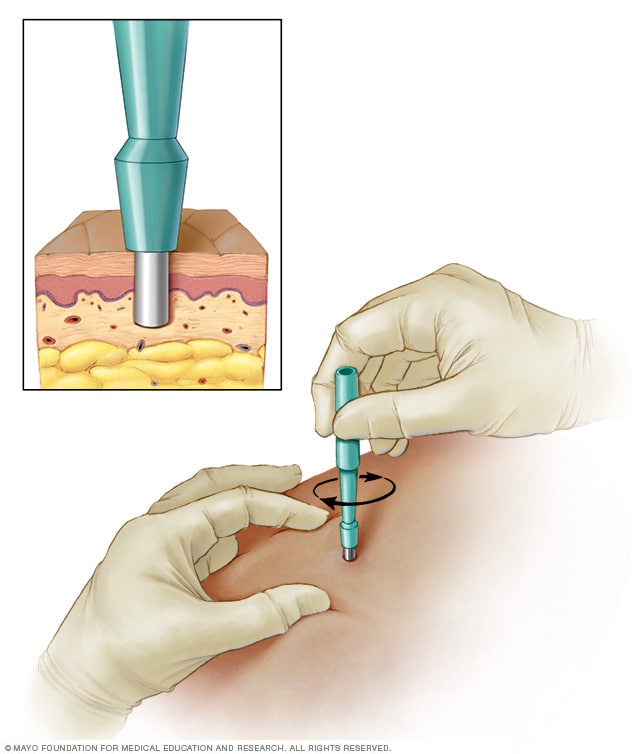
Skin biopsies
Lesion removals
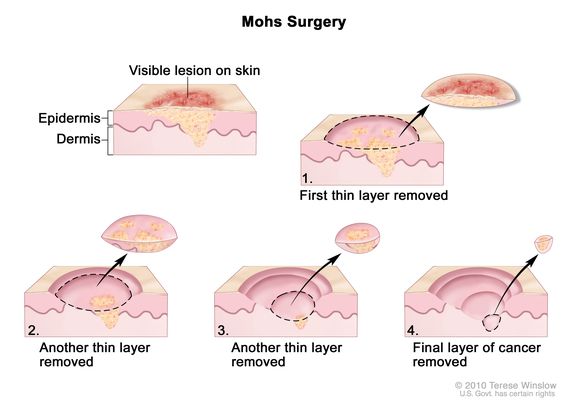
Mohs surgery
Cosmetic vs medical distinction
Proper documentation determines whether a service is reimbursable.
3. Orthopedic Billing
Orthopedic billing often involves:
Fracture care
Joint replacements
Physical therapy
Imaging services
Key billing considerations:
Global surgical periods
Durable Medical Equipment (DME)
Multiple procedure reductions
Modifier accuracy
4. Mental Health & Behavioral Health Billing
Mental health billing includes:
Individual therapy
Group therapy
Psychiatric evaluations
Telehealth sessions
Special challenges:
Authorization requirements
Time-based CPT codes
Telehealth billing regulations
Parity law compliance
5. Pediatrics Billing
Pediatric billing involves:
Well-child visits
Immunizations
Developmental screenings
Preventive services
Preventive care coding is critical to ensure proper reimbursement.
6. Obstetrics & Gynecology (OB/GYN) Billing
OB/GYN billing is complex due to:
Global maternity packages
Delivery codes
Ultrasound billing
High-risk pregnancy documentation
Precise tracking of prenatal visits is required for accurate claims.
7. Internal Medicine Billing
Internal medicine practices treat a wide range of chronic and acute conditions.
Key billing factors:
Evaluation & Management (E/M) codes
Chronic care management (CCM)
Preventive services
Medicare compliance
Frequent updates in E/M guidelines require experienced billing professionals.
8. Radiology Billing
Radiology billing requires:
Professional vs technical component separation
Imaging modifiers
Prior authorizations
Accurate diagnosis support
Errors can result in high-value claim denials.
Key Benefits of Specialty Medical Billing Services
1. Higher Revenue Collection
Specialty-focused billing reduces coding errors and maximizes reimbursements.
2. Reduced Claim Denials
Experienced billers understand payer-specific rules for each specialty.
3. Compliance Assurance
Maintains HIPAA compliance and Medicare regulations.
4. Faster Reimbursement Cycles
Clean claims result in quicker payments.
5. Improved Reporting & Analytics
Specialty billing includes detailed performance metrics.
CareMSO provides customized reporting tailored to specialty-specific KPIs.
Challenges in Specialty Medical Billing
Even experienced providers struggle with:
Constant CPT and ICD-10 updates
Changing payer policies
Pre-authorization requirements
Telehealth billing regulations
Audits and compliance risks
Without expert management, these challenges can significantly impact revenue.
How CareMSO Supports Medical Billing Specialties in the USA
CareMSO offers end-to-end specialty billing services, including:
Specialty-certified coders
Claims submission and tracking
Denial management
Accounts receivable follow-up
Credentialing support
Compliance audits
Revenue cycle management (RCM)
By partnering with CareMSO, healthcare providers can focus on patient care while experts handle the financial workflow.
How to Choose the Right Specialty Billing Partner
When selecting a billing company in the USA, consider:
Specialty expertise
U.S. compliance knowledge
Transparent reporting
Technology integration (EHR/EMR compatibility)
Proven denial reduction rates
HIPAA-compliant processes
CareMSO checks all these boxes, offering scalable solutions for small practices and large healthcare organizations.
Future Trends in Medical Billing Specialties (USA Market)
The healthcare landscape continues to evolve. Emerging trends include:
AI-driven coding assistance
Telehealth expansion
Value-based care reimbursement
Automation in claim scrubbing
Data analytics for revenue optimization
Specialty-focused billing services are adapting rapidly to meet these demands.
FAQs About Medical Billing Specialties
1. What are medical billing specialties?
Medical billing specialties refer to billing services customized for specific healthcare disciplines such as cardiology, dermatology, orthopedics, and more.
2. Why is specialty billing important?
Each specialty has unique coding and reimbursement rules. Proper expertise reduces denials and increases revenue.
3. How does specialty billing improve revenue?
Accurate coding, correct modifiers, and payer compliance result in higher reimbursement rates and fewer rejected claims.
4. Is specialty billing required for small practices?
Yes. Even small practices benefit from specialty expertise to ensure accurate and compliant billing.
5. Does CareMSO handle multiple specialties?
Yes. CareMSO provides tailored billing solutions across various medical specialties in the USA.
6. How can I reduce claim denials in my specialty?
By using certified specialty coders, maintaining accurate documentation, and following payer-specific rules.
7. Is telehealth billing different by specialty?
Yes. Telehealth coding requirements vary by specialty and payer guidelines.
Conclusion
Medical billing specialties are essential for modern healthcare providers in the USA. Each medical discipline comes with unique coding complexities, payer requirements, and compliance challenges. Without specialized billing expertise, practices risk revenue loss, denied claims, and regulatory penalties.
Partnering with an experienced billing provider like CareMSO ensures accuracy, compliance, and optimized revenue cycle management. Whether you operate a cardiology clinic, dermatology practice, mental health center, or multi-specialty facility, specialty-focused billing services can transform your financial performance.
If you're ready to maximize reimbursements and streamline operations, CareMSO is your trusted partner in specialty medical billing solutions across the United States.